According to the American Diabetes Association, about 15.7 million people (5.9 percent of the United States population) have diabetes. Nervous system damage (also called neuropathy) affects about 60 to 70 percent of people with
diabetes and is a major complication that may cause diabetics to lose feeling in their feet or hands.
Foot problems are a big risk in diabetics. Diabetics must constantly monitor their feet or face severe consequences, including amputation. The diabetic foot is one of the most common conditions we treat in our six offices: Rocky
Hill CT, Bristol CT, Newington CT, Glastonbury CT, Middletown CT, and Kensington CT. Our four podiatrists, Dr. Jeffrey S. Kahn, Dr. Richard E. Ehle, Dr. Craig M. Kaufman, and Dr. Ayman M. Latif are highly trained in treating the
diabetic foot.
With a diabetic foot, a wound as small as a blister from wearing a shoe that's too tight can cause a lot of damage. Diabetes decreases blood flow, so injuries are slow to heal. When your wound is not healing, it's at risk for
infection. As a diabetic, your infections spread quickly. If you have diabetes, you should inspect your feet every day. Look for puncture wounds, bruises, pressure areas, redness, warmth, blisters, ulcers, scratches, cuts and nail
problems. Get someone to help you, or use a mirror.
Here's some basic advice for taking care of your feet:
- Always keep your feet warm.
- Don't get your feet wet in snow or rain.
- Don't put your feet on radiators or in front of the fireplace.
- Don't smoke or sit cross-legged. Both decrease blood supply to your feet.
- Don't soak your feet.
- Don't use antiseptic solutions, drugstore medications, heating pads or sharp instruments on your feet.
- Trim your toenails straight across. Avoid cutting the corners. Use a nail file or emery board. If you find an ingrown toenail, contact our office.
- Use quality lotion to keep the skin of your feet soft and moist, but don't put any lotion between your toes.
- Wash your feet every day with mild soap and warm water.
- Wear loose socks to bed.
- Wear warm socks and shoes in winter.
- When drying your feet, pat each foot with a towel and be careful between your toes.
- Buy shoes that are comfortable without a "breaking in" period. Check how your shoe fits in width, length, back, bottom of heel, and sole. Avoid pointed-toe styles and high heels. Try to get shoes made with leather upper material and deep toe boxes. Wear new shoes for only two hours or less at a time. Don't wear the same pair everyday. Inspect the inside of each shoe before putting it on. Don't lace your shoes too tightly or loosely.
- Choose socks and stockings carefully. Wear clean, dry socks every day. Avoid socks with holes or wrinkles. Thin cotton socks are more absorbent for summer wear. Square-toes socks will not squeeze your toes. Avoid stockings with elastic tops.
Diabetic Complications and Amputation Prevention
People with diabetes are prone to having foot problems, often because of two complications of diabetes: nerve damage (neuropathy) and
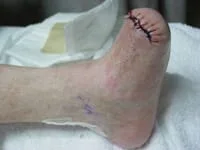
Having diabetes increases the risk of developing a wide range of foot problems. Furthermore, with diabetes, small foot problems can turn into serious complications.
Diabetes-related Foot and Leg Problems
- Infections and ulcers (sores) that don't heal. An ulcer is a sore in the skin that may go all the way to the bone. Because of poor circulation and neuropathy in the feet, cuts or blisters can easily turn into ulcers that become infected and won't heal. This is a common- and serious- complication of diabetes and can lead to a loss of your foot, your leg, or your life.
- Corns and calluses . When neuropathy is present, you can't tell if your shoes are causing pressure and producing corns or calluses. Corns and calluses must be properly treated or they can develop into ulcers.
- Dry, cracked skin. Poor circulation and neuropathy can make your skin dry. This may seem harmless, but dry skin can result in cracks that may become sores and can lead to infection.
- Nail disorders. Ingrown toenails (which curve into the skin on the sides of the nail) and fungal infections can go unnoticed because of loss of feeling. If they are not properly treated, they can lead to infection.
- Hammertoes and bunions. Nerve damage affecting muscles can cause muscle weakness and loss of tone in the feet, resulting in hammertoes and bunions. If left untreated, these deformities can cause ulcers.
- Charcot foot. This is one of the most serious foot problems you can face. It warps the shape of your foot when your bones fracture and disintegrate, and yet you continue to walk on it because it doesn't hurt. Diabetic foot ulcers and early phases of Charcot fractures can be treated with a total contact cast. The shape of your foot molds the cast. It lets your ulcer heal by distributing weight and relieving pressure. If you have Charcot foot, the cast controls your foot's movement and supports its contours if you don't put any weight on it. To use a total contact cast, you need good blood flow in your foot. The cast is changed every week or two until your foot heals. A custom-walking boot is another way to treat your Charcot foot. It supports the foot until all the swelling goes down, which can take as long as a year. You should keep from putting your weight on the Charcot foot. Surgery is considered if your deformity is too severe for a brace or shoe.
- Poor blood flow. In diabetes, the blood vessels below the knee often become narrow and restrict blood flow. This prevents wounds from healing and may cause tissue death.
What Your Foot and Ankle Surgeon Can Do
Your foot and ankle surgeon can help wounds heal, preventing amputation. There are many new surgical techniques available to save feet and legs, including joint reconstruction and wound healing technologies. Getting regular foot checkups and seeking immediate help when you notice something can help small problems from worsening. Your foot and ankle surgeon works together with other health care providers to prevent and treat complications from diabetes.
Your Proactive Measures
You play a vital role in reducing complications. Follow these guidelines and contact your foot and ankle surgeon if you notice any problems:
- Inspect your feet daily: If your eyesight is poor, have someone else do it for you.
- Skin or nail problems: Look for cuts, scrapes, redness, drainage, swelling, bad odor, rash, discoloration, loss of hair on toes, injuries, or nail changes (deformed, striped, yellowed or discolored, thickened, or not growing).
- Signs of fracture: If your foot is swollen, red, hot, or has changed in shape, size, or direction, see your foot or ankle surgeon immediately.
- Don't ignore leg pain: Pain in the leg that occurs at night or with a little activity could mean you have a blocked artery. Seek care immediately.
- Nail cutting: If you have nail problems, hard nails, or reduced feeling in your feet, your toenails should be properly trimmed.
- No "bathroom surgery: Never trim calluses or corns yourself, and never use over-the-counter medicated pads.
- Keep floors free of sharp objects: Make sure there are no needles, insulin syrines, or other sharp objects on the floor.
- Don't go barefoot: Wear shoes, indoors and outdoors.
- Check shoes and socks: Shake out your shoes before putting them on. Make sure your socks aren't bunched up.
- Have your circulation and sense of feeling tested: Your foot and ankle surgeon will perform tests to see if you've lost any feeling or circulation. Our office offers PAD (Peripheral Artery Disease) testing.
When Is Amputation Necessary?
Even with preventative care and prompt treatment of infection and complications, there are instances when amputation is necessary to remove infected tissue, save a limb, or even save a life.
Diabetic Peripheral Neuropathy
Diabetic neuropathy is nerve damage caused by diabetes. When it affects the arms, hands, legs, and feet it is known as diabetic peripheral neuropathy. Diabetic peripheral neuropathy is different from peripheral arterial disease (poor circulation), which affects the blood vessels rather than the nerves.
Three groups of nerves can be affected by diabetic neuropathy:
- Sensory nerves , which enable people to feel pain, temperature, and other sensations
- Motor nerves , which control the muscles and give them their strength and tone
- Automatic nerves , which allow the body to perform certain involuntary functions, such as sweating.
Diabetic peripheral neuropathy doesn't emerge overnight. Instead, it usually develops slowly and worsens over time. Some patients have this condition long before they are diagnosed with diabetes. Having diabetes for several years may increase the likelihood of having diabetic neuropathy.
The loss of sensation and other problems associated with nerve damage make a patient prone to developing skin ulcers (open sores) that can become infected and may not heal. This serious complication of diabetes can lead to a loss of a foot, a leg, or even life.
Causes
The nerve damage that characterizes diabetic peripheral neuropathy is more common in patients with poorly managed diabetes. However, even diabetic patients who excellent blood sugar (glucose) control can develop diabetic neuropathy. There are several theories as to why this occurs, including the possibilities that high blood glucose or constricted blood vessels produce damage to the nerves.
As diabetic peripheral neuropathy progresses, various nerves are affected. These damaged nerves can cause problems that encourage development of ulcers. For example:
- Deformities (such as bunions or hammertoes) resulting from motor neuropathy may cause shoes to rub against toes, creating a sore. The numbness caused by sensory neuropathy can make the patient unaware that this is happening.
- Because of numbness, a patient may not realize that he or she has stepped on a small object and cut the skin.
- Cracked skin caused by autonomic neuropathy, combined with sensory neuropathy numbness and problems associated with motor neuropathy can lead to developing a sore.
Symptoms
Depending on the type(s) of nerves involved, one or more symptoms may be present in diabetic peripheral neuropathy.
For sensory neuropathy:
- Numbness or tingling in the feet
- Pain or discomfort in the feet or legs, including prickly, sharp pain, or burning feet
For motor neuropathy:
- Muscle weakness and loss of muscle tone in the feet and lower legs
- Loss of balance
- Changes in foot shape that lead to areas of increased pressure
For autonomic neuropathy:
- Dry feet
- Cracked skin
Diagnosis
To diagnose diabetic peripheral neuropathy, the foot and ankle surgeon will obtain the patient's history of symptoms and will perform simple in-office tests on the feet and legs. This evaluation may include assessment of the patient's reflexes, ability to feel light touch, and ability to feel vibration. In some cases, additional neurologic tests may be ordered.
Treatment
First and foremost, treatment of diabetic peripheral neuropathy centers on control of the patient's blood sugar level. In addition, various options are used to treat the painful symptoms.
Medications are available to help relieve specific symptoms, such as tingling or burning. Sometimes a combination of different medications is used.
In some cases, the patient may also undergo physical therapy to help reduce balance problems or other symptoms.
Prevention
The patient plays a vital role in minimizing the risk of developing diabetic peripheral neuropathy and in preventing its possible consequences. Some important preventative measures include:
- Keep blood sugar levels under control.
- Wear well-fitting shoes to avoid getting sores.
- Inspect your feet every day. If you notice any cuts, redness, blisters, or swelling, see your foot and ankle surgeon right away. This can prevent problems from becoming worse.
- Visit your foot and ankle surgeon on a regular basis for an examination to help prevent the foot complications of diabetes.
- Have periodic visits with your primary care physician or endocrinologist. The foot and ankle surgeon works together with these and other people to prevent and treat complications from diabetes.
More Reading
Diabetes is such a large topic, we have an entire blog for it! Visit http://diabeticfootct.blogspot.com/ for weekly updates and recipes.

